By Nancy Simpkins
What single thing can improve your appearance, reduce your risk of suffering chronic back pain and headaches, improve your circulation and digestion, and reduce your stress levels? No, it’s not a miracle drug. It’s good posture.
What is good posture?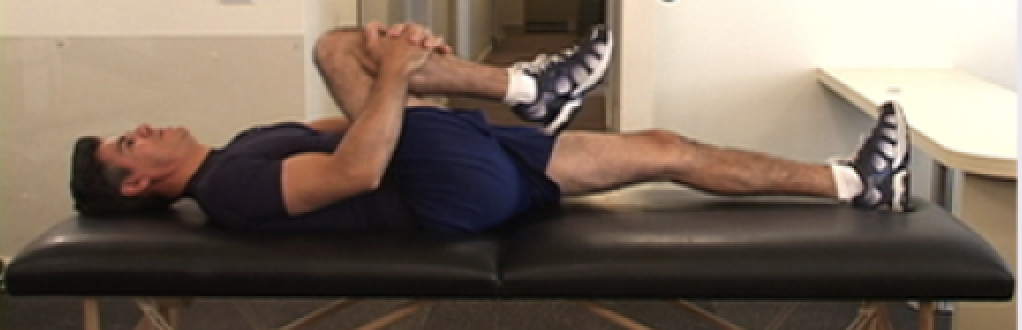
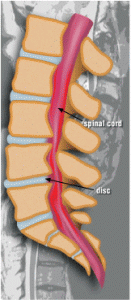
Good posture keeps your bones properly aligned, reducing the strain on your muscles and joints. When your posture is correct, your spine will curve slightly forward at the neck, slightly backward in the upper back, and slightly forward in the lower back. These are the cervical, thoracic and lumbar curves. Strong and flexible muscles in the abdomen, hips and legs make it easier to maintain good posture.
Bad posture can increase pain
Poor posture can cause misalignment of the joints, resulting in excessive wear and tear that leads to arthritis. Muscles become imbalanced, with some growing stronger and tighter, while others grow weaker and overstretched. Imbalances can put pressure on nerves, causing pain. Excessive pressure on the sciatic nerve causes pain in the back and legs, and misalignment of the cervical spine can lead to headaches. Neck pain frequently results from poor posture. For example, studies have shown that the forward head position common when using a smartphone can lead to neck pain.
Poor posture can also compress blood vessels, interfering with normal circulation. When a slumped sitting posture compresses the abdomen, stomach contents may back up into the esophagus and cause gastroesophageal reflux (GERD).
Can physical therapy correct your posture?
Causes of bad posture include weak muscles, poor flexibility, improper sitting and standing habits, obesity, pregnancy, and wearing high-heeled shoes. Physical therapists can evaluate and treat problems with posture. Treatment will usually include exercises to strengthen weak muscles and stretch tight ones, so that the body can achieve proper alignment.
One patient developed severe pain and tingling down her right arm, radiating to the hand. She came to see Hector Mayo, clinical director at Grand Central Physical Therapy and Hand Therapy. A discussion of her symptoms revealed that the pain had begun within weeks after she started working from home.
“The poor ergonomics in her home office had worsened her posture, leading to cervical radiculitis,” Mayo explained. This refers to a pinched nerve, and it was causing the pain. “Using manual traction, electrical stimulation, and therapeutic exercise, I was able to reduce her symptoms. I also advised her how to set up her monitor and chair so she was sitting with good posture, and she continued to do the postural exercises I showed her. She made a complete recovery.”
 By Nancy Simpkins
By Nancy Simpkins