When lumbar strain causes back pain, strengthening the core muscles can help. Trunk rotation exercises are one way to make the core muscles stronger.
Uncategorized
Baker’s Cysts
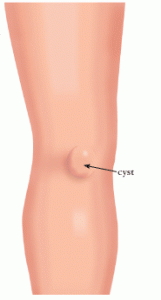 A Baker’s cyst, also called a popliteal cyst, is a fluid-filled lump behind the knee. It is named after William Morrant Baker, the doctor who first described it. The cyst occurs when the popliteal bursa, a soft pouch behind the knee, accumulates excess fluid and expands. It may feel like a water-filled balloon.
A Baker’s cyst, also called a popliteal cyst, is a fluid-filled lump behind the knee. It is named after William Morrant Baker, the doctor who first described it. The cyst occurs when the popliteal bursa, a soft pouch behind the knee, accumulates excess fluid and expands. It may feel like a water-filled balloon.
The fluid in a Baker’s cyst is synovial fluid, which normally lubricates the joint. Excess fluid can build up after an injury such as a tear of the meniscal cartilage in the knee. These cysts are also associated with knee arthritis.
Symptoms may include stiffness, pain, swelling, or a decrease in range of motion. A cyst that ruptures may also cause bruising on the back of the knee and calf. Sometimes a blood clot can be confused with a ruptured Baker’s cyst, but in the case of a blood clot, immediate treatment is required. If your calf is red and swollen, you should seek medical attention.
Baker’s cysts may go away without treatment, but large and painful cysts are usually treated. If you have a Baker’s cyst, a physical therapist can teach you range of motion and strengthening exercises to reduce symptoms and maintain knee function. Your therapist may also apply ice or a compression bandage to reduce swelling. Your doctor may also reduce swelling with a corticosteroid injection or by draining the fluid from the cyst. If the cyst is caused by torn cartilage or arthritis, surgery may be recommended.
Shin Splints
By Lisa Gemmel, MPT
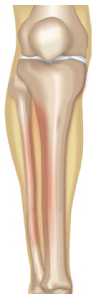 Shin splints is a disorder affecting the muscle-tendon unit in the lower leg. Symptoms include pain, soreness or tenderness in the front of the lower leg. The condition is brought on by overuse, and while it can be caused by many activities, the most common one is running. People with low arches have a higher than normal risk of shin splints.
Shin splints is a disorder affecting the muscle-tendon unit in the lower leg. Symptoms include pain, soreness or tenderness in the front of the lower leg. The condition is brought on by overuse, and while it can be caused by many activities, the most common one is running. People with low arches have a higher than normal risk of shin splints.
Treatment should begin with stopping the activity causing the pain and trying an alternative form of training, such as non-impact underwater running, using an elliptical machine or cycling. Ice and anti-inflammatory medications such as ibuprofin can also help. If these measures are not successful in alleviating the pain, or if the pain gets worse, it’s time to seek medical attention from an orthopedist.
After ruling out other causes of pain in the area, such as a stress fracture or compartment syndrome, the orthopedist will refer you to a physical therapist. The therapist will evaluate you and identify which mechanical stresses are causing the problem. The affected muscle can then be strengthened and conditioned by performing specific exercises and stretches. Heat applied before exercise increases blood flow and warms up the muscles, and ice is used after exercise to reduce inflammation. Orthotics or a change of footwear may be recommended to help cushion the shin and put your foot in the correct alignment, which reduces the strain on the muscle.
Total Knee Replacement
By Nancy Simpkins
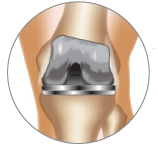 When arthritis in the knee causes severe pain or disability that is not improved by conservative treatments, your doctor may recommend surgery to replace the joint. In total knee replacement surgery, damaged cartilage is removed, and a metal or plastic joint is attached to the femur (thigh bone), tibia (shin) and patella (knee cap).
When arthritis in the knee causes severe pain or disability that is not improved by conservative treatments, your doctor may recommend surgery to replace the joint. In total knee replacement surgery, damaged cartilage is removed, and a metal or plastic joint is attached to the femur (thigh bone), tibia (shin) and patella (knee cap).
Minimally invasive total knee replacement
Some orthopedic surgeons do quadriceps-sparing minimally invasive total knee replacement, which requires a smaller incision than in traditional surgery, and eliminates the need to cut the quadriceps tendon and muscles, and to dislocate the kneecap. Patients benefit from a shorter hospital stay, shorter recovery time and a smaller scar.
Physical therapy after knee replacement surgery
After knee replacement surgery, your physical therapist can teach you exercises that strengthen the muscles in the knee and increase the range of motion in the joint. Physical therapy can also help reduce pain and swelling. Some patients may need to relearn good standing and walking techniques. Many patients with knee pain develop a habit of using the hips to stand up from a chair, which increases the risk of falling and could lead to future knee osteoarthritis. After knee replacement surgery eliminates the pain, a physical therapist can train these patients to use their quadriceps muscles instead.
How long does a total knee replacement last?
In addition to improving function in the knee, exercise can help control weight, which is important since excess weight can reduce the life of the new joint. When knee replacement began in the 1970’s, the life of the replacement joint was estimated at 10 years. Current replacement joints are expected to last closer to 20 years.
Dupuytren’s Disease
By Marianne Pilgrim, OTR/L, CHT
 Dupuytren’s disease is a disorder of the connective tissue in the palm of the hand. The disease usually starts with nodules that progress to tendon-like bands. These eventually pull the fingers, particularly the ring and small fingers, into a bent position toward the palm. It becomes difficult to straighten or spread the fingers, limiting activities such as shaking hands, putting hands into pockets or gloves, and holding large objects.
Dupuytren’s disease is a disorder of the connective tissue in the palm of the hand. The disease usually starts with nodules that progress to tendon-like bands. These eventually pull the fingers, particularly the ring and small fingers, into a bent position toward the palm. It becomes difficult to straighten or spread the fingers, limiting activities such as shaking hands, putting hands into pockets or gloves, and holding large objects.
The exact cause of Dupuytren’s disease remains unknown. There is a strong genetic basis, with a family history in 25% of cases. The disease is most common among Caucasian males of Northern European descent, and is less prevalent among people with Asian or African ancestry. There is also a higher incidence among smokers, alcoholics, diabetics and epileptics. The average age of onset is 45 years for males and 60 years for females. Dupuytren’s disease typically takes 10 years to develop from onset to the stage where correction is needed.
Stress Fractures
By Nancy Simpkins
 A stress fracture is a small crack in a bone, occurring most often in the lower leg or foot. These fractures are usually caused by overuse, particularly among participants in sports such as tennis, running, gymnastics and basketball.
A stress fracture is a small crack in a bone, occurring most often in the lower leg or foot. These fractures are usually caused by overuse, particularly among participants in sports such as tennis, running, gymnastics and basketball.
Bones break down and repair themselves in response to stress, and the muscles also act as shock absorbers to protect the bones. When the muscles become fatigued, extra force may be transmitted to the bones. If an athlete increases the amount or intensity of activity more quickly than the bones can rebuild themselves, a stress fracture will develop.
Poor nutrition that diminishes bone health can increase the risk of stress fractures, and having leg-length discrepancies, flat feet or high arches increases the risk as well. People with osteoporosis can experience stress fractures from activities of daily living.
The symptoms of a stress fracture are pain and swelling that increases with activity. Treatment includes rest, ice and pain relievers. Some experts recommend acetaminophen because non-steroidal anti-inflammatory medicines may interfere with bone healing. For severe stress fractures in the foot, a splint, cast, walking boot or crutches may be necessary, or a surgeon may need to insert a pin to hold the bone together. Patients recovering from stress fractures can benefit from physical therapy to learn exercises that improve strength and stability.

